Breathing easy, at last – broadening the path to lung transplant for patients with Cystic Fibrosis
11-year-old Lizzy was able to receive a life-saving transplant thanks to improved technology and Stanford expertise, along with her own determination and an extraordinary community of support.
By Erin Digitale
When Lizzy Highstreet could finally speak to her parents after an important surgery last July, she had a pressing question for her dad: “Why don’t I have oxygen?”
“What do you mean?” Aaron Highstreet said. “You got lungs!”
Lizzy, 11, had temporarily forgotten why she’d had surgery: Following more than a month in the hospital with severe complications of cystic fibrosis, she had received a lung transplant July 18 at Lucile Packard Children’s Hospital Stanford.
“It was pretty amazing to walk in there and see her just easily breathing, not struggling,” said Tina Highstreet, Lizzy’s mom.
Lizzy followed an unusual and difficult path to transplant. Before the surgery, she was kept alive for 37 days by extracorporeal membrane oxygenation, essentially the “lung” function of a heart-lung machine. Her doctors believe it is among the longest periods that ECMO has been used as a bridge to lung transplant for a child in the United States.
It was the culmination of a tremendous team effort — boosted by the expertise of Packard Children’s caregivers, the power of recent technical advances, the strength of Lizzy’s family and community, and the extraordinary grit and determination of the patient herself.
“The remarkable thing about Lizzy is that even though her lungs were so bad, she had very unique mental fortitude to be calm in difficult scenarios,” said critical care physician Bereketeab Haileselassie, MD, who looked after Lizzy in the Packard Children’s pediatric intensive care unit.
Fighting complications
In the years before her transplant, Lizzy experienced a series of complications of cystic fibrosis. The genetic disease impairs the body’s secretory glands, making lung mucus stickier than normal and leaving patients vulnerable to respiratory infections.
To manage a rare, chronic lung infection, Lizzy saw a team at Valley Children’s Hospital in Madera, Calif. The hospital partners with Stanford Medicine Children’s Health specialists, including pediatric pulmonologist Carlos Milla, MD, who cared for Lizzy in Madera and during her inpatient stays at Packard Children’s Hospital. Although her health fluctuated, Lizzy could usually attend school and church in her hometown of Visalia, Calif.; go on beach trips with her three siblings and their cousins; and play her favorite sports, volleyball and soccer.
But, after hospitalizations in late 2017 and early 2018, it was clear she would need a lung transplant. By early June she was back in Packard Children’s again, being placed on a ventilator.
“It was really tough, the night they intubated her, to see her struggle to breathe so much,” Tina said. She and Aaron relied on their Christian faith at this moment and many others throughout the long hospitalization. “When there were things that felt out of our control, we were praying for God to provide opportunities or answers for her,” Tina said.
After a week on the ventilator, Lizzy’s physicians switched her to ECMO, using a neck catheter. Instead of blowing air into her lungs, the ECMO equipment carried Lizzy’s blood out of her body via plastic tubing. The equipment removed carbon dioxide, added oxygen and returned Lizzy’s blood to her body.
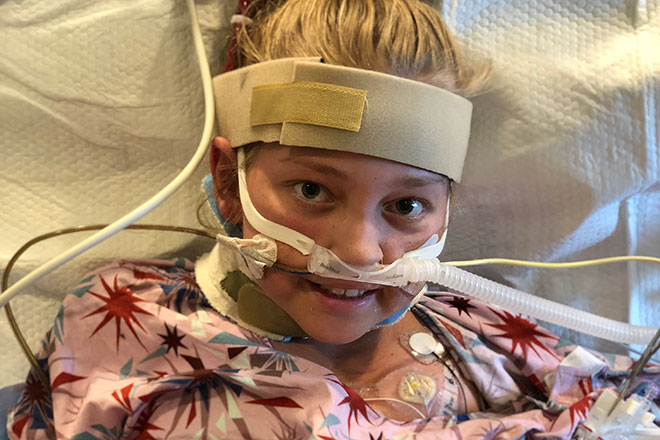
Lizzy smiling despite the cumbersome neck cannula that she was attached to. Photo courtesy of Highstreet family.
In the past, ECMO wouldn’t have been considered for a patient awaiting lungs. ECMO patients were traditionally sedated, losing muscle strength they would need to recover from a transplant. And the plastic tubing inside the machines increased the risk of blood clotting and immune reactions, making it hard to match a patient to a donor organ.
But in recent years, ECMO equipment has improved. The tubing circuits are smaller and coated in anticoagulant, reducing the risk of clotting. Critical-care specialists have also begun using ECMO without sedation. In the last year, three Packard Children’s patients with lung disease who did not need transplants each spent several weeks on ECMO, allowing their lungs to rest and recover. Those successes gave the team the confidence to move forward with Lizzy’s more difficult case.
“As long as the patient is moving around, they can be a good candidate for lung transplant,” said cardiothoracic surgeon Katsuhide Maeda, MD, who performed Lizzy’s transplant.
It wasn’t easy: Moving Lizzy around with the neck cannula required 12 to 15 people.
“But Lizzy took it in good stride and worked with us to keep her muscles strong,” said Haileselassie. “It was amazing how much she could do with a full ECMO circuit attached to her neck.”
Still, the wait for donor lungs for a child can be several months. No one was sure if a match could be found soon enough.
Courage for a difficult wait
During Lizzy’s hospitalization, the Highstreets’ Visalia church organized a prayer drive. Participants posted Instagram photos of themselves with raised arms and the hashtag #LizzyBrave, “holding us up as we were fighting the battle,” Tina Highstreet said. Lizzy’s team of Packard Children’s caregivers also took a group photo of themselves holding up their hands and posted it in her hospital room.

Members of Lizzy’s Packard Children’s care team putting their hands up for the #LizzyBrave campaign. Photo courtesy of the Highstreet family.
As the campaign spread, Lizzy loved mapping its progress. “We got all 50 states and eight countries,” she said. “We put a heart in every one as we found out somebody was praying for me there.”
In early July, when Lizzy needed a blood transfusion to help reduce the number of minor antigens that her body was exposed to, family and friends used the #LizzyBrave hashtag to ask for blood donations. “About 60 friends and family came to Stanford to donate blood,” Tina said.
The Highstreets also drew strength from the close ties they formed with Lizzy’s caregivers.
“Her family is as remarkable as she is,” said Haileselassie. “They were obviously frightened, but they came at this with a very positive mental construct. Every time a new provider came on, they said, ‘Welcome to Lizzy’s team.’ They coped with the stresses by rolling up their sleeves.”
A dangerous hemorrhage

On July 13, leaving Aaron at Packard Children’s with Lizzy, Tina went to Visalia to catch up on things at home. The next morning, on the drive back, Tina’s phone rang. A blood vessel had broken in Lizzy’s lungs, likely due to worsening necrosis. She was losing a lot of blood.
Tina arrived in Lizzy’s hospital room just in time to “tell her I loved her, to be brave, to fight, before they sedated her,” she said. “We didn’t know if they could stop the bleeding.”
The medical team intubated Lizzy again and controlled her bleeding, but the incident heightened everyone’s worry about whether Lizzy would survive to receive donor lungs. On the evening of July 16, Lizzy’s ECMO connection was switched to a chest cannula to give her better mobility for long-term use. Early the next morning, Maeda told Lizzy’s parents that she was very weak and would need rehabilitation to regain her strength. Aaron and Tina felt devastated. Would Lizzy live?
Just a few hours later, Maeda came barreling down the hall. “We need to talk,” the surgeon told the parents, herding them into a conference room.
“My stomach fell out,” Tina said. What now? she thought.
But Maeda had good news: Lizzy had matched to donor lungs.
“I remember feeling ecstatic and terrified and relieved and saddened for the family that was giving up their loved one,” said Tina. “It was like being on a rollercoaster of emotions for sure.”
About 40 extended family members, including Lizzy’s grandparents, aunts, uncles and cousins, drove to Palo Alto and waited up until 1:15 a.m. on July 18 for the call confirming that the transplant would go ahead. At 3:30 a.m., Aaron and Tina heard that surgery had begun and Lizzy was receiving her new lungs. After the transplant was complete, Lizzy spent a few days on a ventilator, partly sedated. Her first completely independent breaths were about a week after the surgery; that’s when she could finally ask her dad why she didn’t have oxygen.
Lizzy’s recovery went well. She was discharged to the Ronald McDonald House near the hospital on August 11. She went home to Visalia on October 25, excited to see her friends, her dog, and her very own house.
Before leaving Palo Alto, the Highstreets took a day trip to the beach, a favorite family pastime. Thanks to her new lungs, Lizzy no longer needed a piggyback ride from her dad.
“Watching her walking across the beach with the wind in her hair, able to do that, brought tears to our eyes,” said Tina. “It was a very, very good moment.”

Connect with us:
Download our App: