Notice of West building lobby closure at Lucile Packard Children’s Hospital Stanford
Girl's Massive Airway Tumor Treated Through New Therapy
The lifesaving treatment Isabella Manley received as a baby has allowed her to become a healthy second-grader. The treatment protocol has since been used worldwide to help thousands of others with similar tumors.
For Release: September 4, 2015

In July 2008, when Isabella Manley was just a few weeks old, she developed rapid, raspy breathing.
“She sounded like Darth Vader,” said her mother, Julie Anna.
“Being first-time parents, we didn’t know what to think,” said her dad, Todd. The worried couple took their daughter to the emergency room at a hospital near their Sacramento, California, home.
They couldn’t have guessed what was to come: Isabella would be diagnosed with a tumor so aggressive it would nearly strangle her. And she would become a medical pioneer, among the first to receive a therapy that revolutionized the way these types of tumors are treated.
“The treatment Isabella received is really a marked advancement over what we had before,” said Kay Chang, MD, the pediatric otolaryngologist who cured Isabella’s tumor at Lucile Packard Children’s Hospital Stanford and Stanford Children’s Health. “Today, it’s the standard of care. No one thinks about using other therapies.” Chang is also associate professor of otolaryngology in head and neck surgery at the School of Medicine.
Back in the summer of 2008, Isabella was initially diagnosed with a hemangioma in her airway. The tumor, a mass of blood vessels protruding into her trachea just below her vocal cords, threatened to block the path to her lungs. Hemangiomas often occur on babies’ skin, appearing as red spots that are usually harmless. But the dangerous location of Isabella’s tumor required immediate treatment.
Her doctors in Sacramento tried steroids and laser surgery, then the usual therapies for severe hemangiomas. When those didn’t work, she was referred to Chang for a second surgery to cut out the tumor and reconstruct her trachea. But shortly after this surgery, when Isabella was about 4 months old, her raspy breathing returned. An MRI scan showed why.
Massive Spread
“We found, to our horror, that this hemangioma was massive, surrounding her entire windpipe and also her heart,” Chang said.
“It was becoming tangled into every structure in her neck and crawling down into her chest,” said Mai Thy Truong, MD, a pediatric otolaryngologist now with the hospital’s vascular malformations clinic, which treats children with hemangiomas and other vascular tumors. At the time of Isabella’s treatment, Truong was completing an otolaryngology fellowship under Chang’s tutelage and was closely involved in Isabella’s care.
“When I saw that MRI, I was devastated,” said Truong, who is also a clinical assistant professor of otolaryngology at the School of Medicine. The tumor was too extensive for surgery and was still growing. Truong and Chang feared that it would soon block Isabella’s airway. They were not sure they could save her.
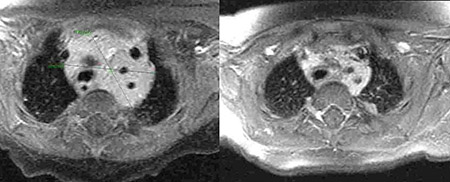
MRI scans show Isabella Manley’s original tumor (left) and how much it had shrunk five days after the first treatment with propranolol. Courtesy of Packard Children's Hospital.
“It was the worst time for us,” Todd said. “The clock was really ticking: her breathing was becoming more labored and the treatments were not working.”
Desperate for answers, Chang recalled a conversation he had heard at a recent medical conference. Some physicians in France had accidentally discovered that a blood pressure medication, propranolol, shrank skin hemangiomas in a few children with high blood pressure who coincidentally had the skin version of the tumor. To Chang’s knowledge, no one had ever used the drug to treat an airway hemangioma, but Isabella’s situation was so dire that he wanted to try. The Manleys agreed.
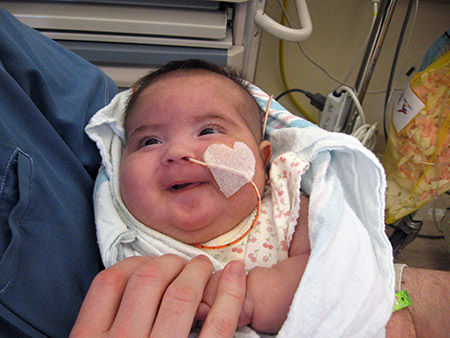
Isabella at Packard Children's in September 2008, before a successful treatment for her airway hemangioma was found. Courtesy of the Manley family.
To everyone’s surprise, Isabella’s breathing improved in the first 24 hours on the medication. A week later, she received another MRI.
“Dr. Chang came and found us and said, ‘You’ve got to see this; the tumor shrunk in half,’” Julie Anna recalled. “We were just beside ourselves.”
After enduring such a long struggle to help Isabella breathe, the Manleys cried happy tears. “It was one of the best days of our lives,” Todd said.
Sharing the news
Chang, meanwhile, couldn’t stop thinking about what the success meant for other children. “I was totally excited,” he said. “It’s rare in medicine that you see something have such a dramatic effect so fast.”
Chang and Truong soon gave a conference presentation at the American Society of Pediatric Otolaryngology about the success of Isabella’s case, making it the first reported instance of a life-threatening airway hemangioma to be successfully treated with propranolol. Other doctors who had also been inspired by the French team began reporting on their use of the medication, too.
Since Isabella was treated in 2008, thousands of children have received propranolol for serious hemangiomas. A recently published series of 207 such cases found that more than 99 percent of the tumors responded to the drug, many as quickly as Isabella’s.
In addition to its speed, propranolol is much safer for children than previous hemangioma treatments. For instance, giving steroids can hinder a child’s growth, and in many cases, steroids only temporarily halt the growth of the tumor. Laser surgery for airway hemangiomas carried the possible side effect of permanent scarring of the vocal cords, which is not a risk with propranolol treatment. Surgeries for large hemangiomas in other locations were often risky and disfiguring, a problem that propranolol has largely solved.
Isabella received propranolol for several months, ending her treatment just before her first birthday. Now a busy second-grader, she loves to read, play soccer, dance and ride her bike.
At a recent checkup, Isabella’s pediatrician told the Manleys that she had been following reports on the use of propranolol in the medical literature. She told them what a difference the drug has made for so many other kids.
“It didn’t hit us until then,” Julie Anna said. “Isabella really is a trailblazer.”
Authors
Erin Digitale
(650) 724-9175
digitale@stanford.edu
About Stanford Medicine Children's Health
Stanford Medicine Children’s Health, with Lucile Packard Children’s Hospital Stanford at its center, is the Bay Area’s largest health care system exclusively dedicated to children and expectant mothers. Our network of care includes more than 65 locations across Northern California and more than 85 locations in the U.S. Western region. Along with Stanford Health Care and the Stanford School of Medicine, we are part of Stanford Medicine, an ecosystem harnessing the potential of biomedicine through collaborative research, education, and clinical care to improve health outcomes around the world. We are a nonprofit organization committed to supporting the community through meaningful outreach programs and services and providing necessary medical care to families, regardless of their ability to pay. Discover more at stanfordchildrens.org.
Connect with us:
Download our App: