Notice of West building lobby closure at Lucile Packard Children’s Hospital Stanford
5 Questions: How Stanford Research is Making MRI Scans Safer for Kids
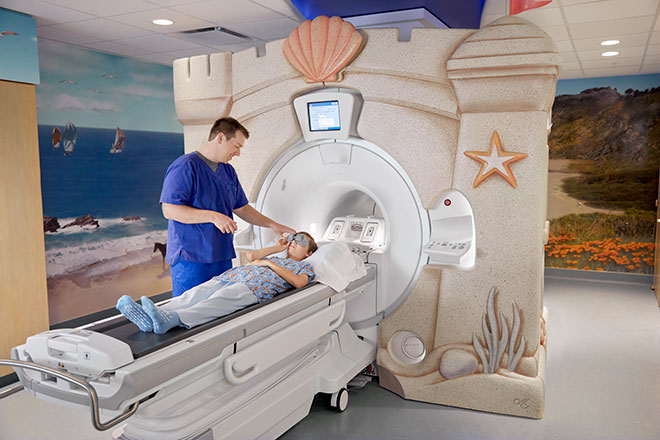
Stanford pediatric radiologist Shreyas Vasanawala is tailoring MRI equipment to children. His work allows young patients to receive faster MRI exams that require less anesthesia.
For release: August 16, 2018
From the Stanford University School of Medicine
When it comes to medical imaging, pediatric radiologist and biomedical engineer Shreyas Vasanawala, MD, PhD, knows that kids aren’t the same as adults.
Vasanawala, MD, PhD, professor of radiology at the School of Medicine, has spent the last 10 years studying how to improve magnetic resonance imaging scans for his smallest, wiggliest patients. Now, he’s putting his MRI innovations to work in the Cynthia Fry Gunn and John A. Gunn Imaging Center at the new Lucile Packard Children’s Hospital Stanford, which opened in December.
1. MRI scans are noninvasive, painless, don’t use radiation and give clear images of soft tissues such as the liver, muscles and tendons, but children who could benefit from MRIs don’t always get them. Why not?
Vasanawala: Magnetic resonance technology is challenging to develop and use. Most of the MRI equipment on the market was designed to meet the needs of adult patients, who receive about 90 percent of MRI exams.
In an MRI scanner, the body is exposed to a very strong magnetic field. The protons in the body’s water molecules align themselves with the magnetic field. We then manipulate them to make them give off radio-frequency signals that are detected by the scanner and translated into a picture.
To produce a clear picture, a traditional MRI scan requires that patients hold very still, sometimes for more than an hour. That’s difficult for young children. Children are also smaller, breathe faster and have higher heart rates — all factors that make the imaging challenges harder from a physics perspective. Kids may be given anesthesia to help them hold still, but that carries its own risks.
Instead, many children receive computed tomography scans, which use powerful X-rays that carry a risk of cancer. Also, for many tissues, CT has less diagnostic power than MRI. We’ve been accepting a suboptimal imaging test for kids because it’s more convenient, faster and doesn’t require anesthesia.
2. As part of your research at Stanford, you’ve been designing MRI equipment especially for children. What improvements have you introduced?
Vasanawala: We’ve invented solutions that have allowed us to eliminate the need for anesthesia in many cases and decreased the depth and duration of anesthesia in others.
We’ve been collaborating with engineers from UC-Berkeley to create new designs and production methods for highly flexible and lightweight MRI signal-receiving coils tailored to children’s bodies. Standard coils are larger than children need, making them unnecessarily heavy and uncomfortable. Larger-than-necessary coils also pick up extra noise or interference, reducing the image quality. Child-size receiver coils increase image clarity and lower scan times.
The smaller coils also greatly enhance the performance of a novel hybrid-imaging technology called PET-MR, which we are now offering to patients in our new imaging center at Packard Children’s Hospital. And the coils are being developed commercially as well.
3. How might these smaller receiver coils also help adult patients?
Vasanawala: There is a whole host of potential applications for adults. Sometimes you can see a lesion on an MRI that you want to biopsy but can’t reach when the area is covered with a big, bulky coil. With the lower-profile equipment, we’ll be able to biopsy through holes in the coil. Also, a light flexible coil is just more comfortable for everyone.
And not every adult is a thin, 6-foot male. The new equipment will help us meet more patients’ needs. For instance, for breast MRI, it’s very helpful to have a form-fitting coil that sits close to the lesions we’re trying to image.
4. You’ve also improved the computing software that processes MRI data. How?
Vasanawala: Joseph Cheng, PhD, an electrical engineer in our group, has taken the lead in creating new image-reconstruction algorithms that work better for kids. We deployed motion-correction strategies that produce sharp images even when a child is moving slightly — this helps address the challenge of kids’ faster heart rates and breathing rates. Simultaneously, to reduce scan times, we implemented novel, high-dimensional imaging and compressed sensing coupled with artificial intelligence. These techniques allow the computer to reconstruct a full MR image from much less raw data. Scans that once took an hour are now complete in 5-10 minutes. This has had a particularly large impact for our cardiac, oncologic and musculoskeletal exams.
5. What most excites you about in the new imaging center at Packard Children’s?
Vasanawala: For the first time, we have an MRI scanner located inside our neurosurgery operating suite. It allows our neurosurgeons to confirm the success of a surgical procedure, such as a tumor resection, before surgery is complete. This saves time by eliminating a separate post-surgical MRI and the risk of needing an immediate repeat surgery. Patients will be spared a second round of anesthesia, hospital stays will be shortened and families will know if the surgical aims have been achieved as soon as their child is out of the operating room.
By the end of 2019, we will have a next-generation MRI scanner with much stronger magnetic field gradients that can be altered at high speed. This enables faster imaging and better image contrasts. Also, this new MRI scanner will come with a noninvasive technology used to kill certain types of tumors using sound waves. Known as MR-guided high-intensity focused ultrasound, it lets us pinpoint abnormal areas in the body, such as some types of tumors, and heat them to destroy the abnormality without cutting into surrounding healthy tissue.
Media Contact:
Erin Digitale
digitale@stanford.edu
(650) 724-9175
About Stanford Medicine Children's Health
Stanford Medicine Children’s Health, with Lucile Packard Children’s Hospital Stanford at its center, is the Bay Area’s largest health care system exclusively dedicated to children and expectant mothers. Our network of care includes more than 65 locations across Northern California and more than 85 locations in the U.S. Western region. Along with Stanford Health Care and the Stanford School of Medicine, we are part of Stanford Medicine, an ecosystem harnessing the potential of biomedicine through collaborative research, education, and clinical care to improve health outcomes around the world. We are a nonprofit organization committed to supporting the community through meaningful outreach programs and services and providing necessary medical care to families, regardless of their ability to pay. Discover more at stanfordchildrens.org.
Connect with us:
Download our App: