Notice of West building lobby closure at Lucile Packard Children’s Hospital Stanford
Synaptive Technology Gives Clearer Paths to Surgical Success
Stanford Medicine Children’s Health is the first pediatric hospital in the world to adopt a powerful new suite of neurosurgery tools that helps brain surgeons conduct cranial surgery more quickly, safely and effectively. The tools, made by Synaptive Medical Inc., feature an ultra-high-resolution camera-telescope/microscope (exoscope) mounted on a robotic arm that automatically tracks a surgeon’s instruments while keeping itself out of the way and providing a continuous, high-resolution, focused, and broad field visible to the entire OR surgical team. BriteMatter Plan, the tool’s presurgical planning software, allows the team to integrate all of a patient’s imaging (MRI, PET, MEG) and other data into a seamless 3D display. It also generates individualized tractography revealing the sensitive white matter highways that control vision, language, motor functions and other key brain activities. Access to all of this data allows physicians to map optimal routes to a tumor or lesion well before surgery.
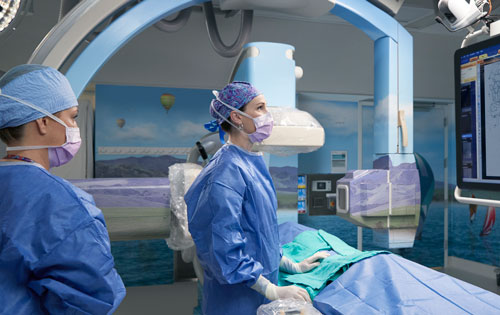
BriteMatter Guide
Synaptive’s intraoperative navigational software, BriteMatter Guide, imports data from the planning software and gives surgeons a dynamic, individualized 3D image, coordinated with the exoscope’s, that helps them steer clear of critical brain structures and the essential tracts that connect them. Our surgeons can now be fully immersed in the 3D brain environment to navigate around the white matter highways that connect critical areas of the brain to maximize safe resection while preserve neurologic function and quality of life.
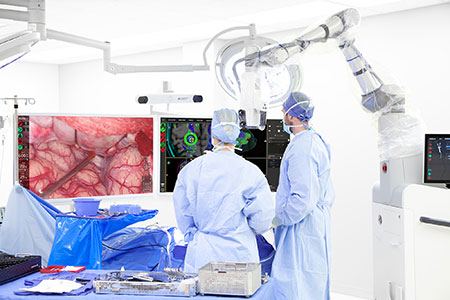
Enabling minimally invasive surgery
Because the tools provide clear visualization of structures in the intact brain, as well as large and vivid images of even a small and deep surgical field, the tools enable minimally invasive surgery with smaller incisions and more precise surgical routes to target deep tumors and lesions, some of which may previously have been considered inoperable. Less invasive surgery often means less time under anesthesia, quicker recovery times, and reduced likelihood of complications. What’s more, clearer real-time imaging and data analysis may enable better identification of a tumor’s or lesion’s margins, allowing surgeons to maximize the resection of tumor or seizure-causing tissue while leaving more healthy brain tissue in place.
Connect with us:
Download our App: