Robotic-Assisted Cardiac Surgery
What is robot-assisted cardiac surgery?
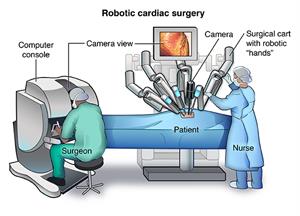
Robot-assisted cardiac surgery is heart surgery done through very small cuts in the chest. The surgeons use tiny instruments and robot-controlled tools to do heart surgery in a way that is much less invasive than open-heart surgery. Robot-assisted cardiac surgery is commonly called robotic cardiac surgery.
Robot-assisted surgeries have been used for a number of different heart-related procedures, including valve surgery, coronary artery bypass, cardiac tissue ablation, heart defect repair, and tumor removal.
Why might I need robot-assisted cardiac surgery?
The main benefit of robot-assisted cardiac surgery is that it is less invasive compared with open-heart surgery. Smaller incisions can mean that you can spend less time in the hospital, heal faster, and return to activities more quickly.
Your healthcare provider will determine if robot-assisted cardiac surgery is right for you. It may be used to:
Repair or replace stiff or leaky heart valves
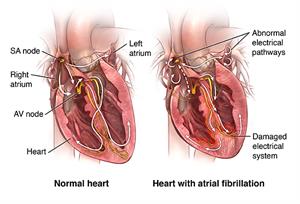
Correct atrial fibrillation, a common type of arrhythmia
Remove a tumor in the heart
Treat congenital heart conditions
To bypass blocked arteries (coronary artery bypass surgery)
Your healthcare provider may have other reasons to recommend robot-assisted cardiac surgery.
What are the risks of robot-assisted cardiac surgery?
One of the main benefits of robot-assisted cardiac surgery is that it has fewer risks than open-heart surgery. The surgeon does not have to cut through the breastbone to open your chest. This removes many of the complications of open-heart surgery.
Robot-assisted cardiac surgery still requires anesthesia and, as with any kind of surgery, there are always risks involved, including:
Heart attack
Stroke
Bleeding
Problems related to the use of anesthesia
Arrhythmias, including a need for a permanent pacemaker
Infection
Death
In some cases, your healthcare provider may not be able to complete the surgery with the robot. If this happens, you would need open-heart surgery. You may have other risks, based on your specific medical condition. Be sure to talk with your healthcare provider about any concerns you have before your procedure.
How do I get ready for robot-assisted cardiac surgery?
To see if you are a good candidate for this procedure, your healthcare provider will review your medical history, and lifestyle, as well as the overall severity of the disease.
Your healthcare provider will explain the procedure to you. Be sure to ask your healthcare provider about any questions you might have.
You will be asked to sign a consent form that gives your permission to do the procedure. Read the form carefully and ask questions if something is unclear.
Along with a complete health history, your healthcare provider may do a physical exam to make sure you are in otherwise good health before you undergo the procedure. You may also have blood tests and other diagnostic tests.
Your healthcare provider may recommend taking an aspirin before the procedure.
Tell your healthcare provider right away if you are pregnant or think you may be.
You should tell your healthcare provider:
If you are sensitive to or are allergic to any medicines, latex, iodine, tape, contrast dyes, and anesthesia (local or general)
About all prescribed and over-the-counter medicines, and herbal supplements that you are taking
If you have a history of bleeding disorders or if you are taking any blood-thinning medicines (anticoagulant), aspirin, or other medicines that affect blood clotting. You may need to stop these medicines before the procedure. Pay attention to which medicines to stop before surgery and when.
If you have a pacemaker or other implanted heart device
If you smoke, stop smoking as soon as possible before the procedure. This will improve your chances for a successful recovery from surgery and your overall health status.
Follow any directions you are given for not eating or drinking before the procedure.
Based on your health condition, your healthcare provider may have other instructions for you.
What happens during robot-assisted cardiac surgery?
Talk with your healthcare provider about the details of your procedure. The following is the general sequence of events that will most likely occur during robot-assisted cardiac surgery:
A healthcare provider with give you anesthesia before the procedure starts. This will cause you to sleep deeply and not feel pain during the surgery. You may receive a sedative before the procedure to help you relax.
Once you are asleep, a breathing tube will be inserted through your throat into your lungs and you will be connected to a ventilator, which will breathe for you during the surgery.
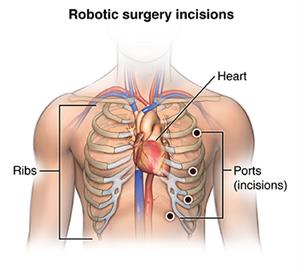
A surgeon will make a series of keyhole-sized cuts (incisions) on the side of your chest. These incisions will align with the openings between your ribs.
You may need to be placed on the heart-lung machine for the procedure.
Depending on the procedure being done, your surgeon will insert several precision-guided robotic arms into these incisions.
These robotic arms hold and manipulate tiny instruments to do the required tasks on the heart or surrounding arteries.
A tiny video camera will be inserted into another incision to provide a magnified, three-dimensional image of the operating site.
The surgeon will control the robotic arms and camera from a console located within the operating room.
Once complete, the surgeon will remove the instruments and close the incisions.
Talk with your healthcare provider about what you will experience during your procedure.
What happens after robot-assisted cardiac surgery?
Once the surgery is done, you will be moved to the recovery area to be monitored. You can expect a relatively short hospital stay to follow, usually half as long as that after conventional open-heart surgery. Your healthcare provider will typically discharge you once your pain is under control, you can keep liquids down without nausea and vomiting, and your lab tests appear near normal or near your baseline before the procedure. Make plans to have someone give you a ride home from the hospital.
You can also expect less scarring on your chest. Open-heart surgery may leave a 10-inch scar on your chest. Robot-assisted cardiac surgery just leaves a few smaller scars on the side of your chest.
After being discharged from the hospital, most people can manage their pain with over-the-counter pain relievers like acetaminophen or ibuprofen. Pain also tends to go away much faster than with open-heart procedures. Remember to take all or your medicines as prescribed.
Your incisions need to be kept clean and dry. Do not use powders, lotions, or ointments on the incision lines as this can irritate the skin and cause prolonged healing and increase the risk for infection. Do not soak the incisions in water until your healthcare provider says it's OK.
You may also return to normal activities more quickly than you would after open-heart surgery. Most people can resume their normal activities after a few weeks. Your healthcare provider will provide specific recommendations for activity.
Your healthcare provider will typically schedule follow-up appointments to check your progress. Tell your healthcare provider right away if any symptoms occur after the procedure, such as chest pain or discomfort. Complications are rare after robot-assisted heart surgery, but they can happen. So it's important to carefully watch out for any symptoms and report them to your healthcare provider.
Next steps
Before you agree to the test or the procedure make sure you know:
The name of the test or procedure
The reason you are having the test or procedure
What results to expect and what they mean
The risks and benefits of the test or procedure
What the possible side effects or complications are
When and where you are to have the test or procedure
Who will do the test or procedure and what that person’s qualifications are
What would happen if you did not have the test or procedure
Any alternative tests or procedures to think about
When and how you will get the results
Who to call after the test or procedure if you have questions or problems
How much you will have to pay for the test or procedure
Connect with us:
Download our App: