Complications of Multiple Pregnancy
Why is multiple pregnancy a concern?
Being pregnant with more than 1 baby is exciting. It is often a happy event for many couples. But multiple pregnancy has higher risks for complications. The most common problems are listed below.
Preterm labor and birth
More than 3 in 5 twins and nearly all higher-order multiples are premature (born before 37 weeks). The higher the number of fetuses in the pregnancy, the greater the risk for early birth. Premature babies are born before their bodies and organ systems have fully matured. These babies are often small, with low birth weights. This means less than 5.5 pounds (2,500 grams). They may need help breathing, eating, fighting infection, and staying warm. Very premature babies are those born before 28 weeks. They are especially vulnerable. Many of their organs may not be ready for life outside the mother's uterus and may be too immature to work well. Many multiple birth babies will need care in a neonatal intensive care unit (NICU).
Gestational high blood pressure
Women with multiple fetuses are more than twice as likely to develop high blood pressure of pregnancy. This health problem often develops earlier and is worse than in pregnancy with one baby. It can also raise the chance of early detachment of the placenta (placental abruption).
Gestational diabetes
Women with multiple fetuses are more likely to get gestational diabetes.
Anemia
Anemia is more than twice as common in multiple pregnancies as in a single birth.
Birth defects
Multiple birth babies have about twice the risk for problems present at birth (congenital) such as spina bifida and other neural tube defects, and problems of the digestive tract and heart.
Miscarriage
A phenomenon called the vanishing twin syndrome is more likely in multiple pregnancies. It's when more than 1 fetus is found, but vanishes (or is miscarried). This often happens in the first trimester. This may come with bleeding. The risk of pregnancy loss is higher in later trimesters as well.
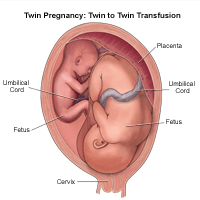
Twin-to-twin transfusion syndrome
Twin-to-twin transfusion syndrome (TTTS) is a condition of the placenta that develops only with identical twins that share a placenta. Blood vessels connect within the placenta and divert blood from one fetus to the other. It happens in about 3 in 20 twins with a shared placenta.
In TTTS, blood is shunted from 1 fetus to the other through blood vessel connections in a shared placenta. Over time, the recipient fetus gets too much blood. This can overload the cardiovascular system and cause too much amniotic fluid to develop. The smaller donor fetus does not get enough blood and has low amounts of amniotic fluid. TTTS can be treated during pregnancy by withdrawing some of the extra fluid with a needle or with surgery on the placenta. Sometimes, the twins may need to be delivered early.
Abnormal amounts of amniotic fluid
Amniotic fluid problems are more common in multiple pregnancies, especially for twins that share a placenta.
Cord entanglement
The umbilical cord for the twins that share amniotic sac can become tangled up. In these cases, the fetuses may need to be monitored often in the third trimester.
Cesarean (C-section) delivery
Abnormal fetal positions raise the chances of a C-section.
Postpartum hemorrhage
The large placental area and over-distended uterus place a mother at risk for bleeding after giving birth.
Connect with us:
Download our App: