Contact us
To learn more about Project ECHO®, call or email the Clinic Coordinator, Lauren Figg, LMSW.
Notice of West building lobby closure at Lucile Packard Children’s Hospital Stanford
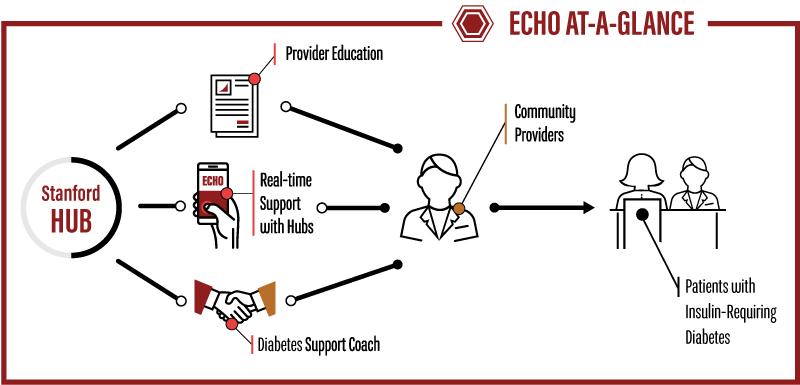
The goal of ECHO Diabetes is to increase the capacity of primary care providers (PCPs) and clinics to empower and safely and effectively manage underserved patients with insulin-requiring diabetes who do not receive routine specialty care. The program was developed in response to the success of the ECHO T1D program, which was the first of its kind to tackle complex diabetes in the primary care setting.
Connect with us:
Download our App: